Summary (TL;DR)
Patient-centred care means more than treating illness. According to Mead & Bower’s Five Dimensions (2000), it involves recognising the biopsychosocial context, respecting the patient as a person, sharing power in decisions, building therapeutic alliances, and acknowledging the doctor as a person. Carolina’s story illustrates how each dimension plays out in real life. With AI, patients can access clearer explanations, reduce uncertainty, and contribute meaningfully to shared decisions. Far from replacing clinicians, AI strengthens these five dimensions by giving both patient and doctor the same high-quality foundation for care.
1. Introduction
In our first article of this series, we explored how Carolina Millon moved from being a passive recipient of care to an active partner in her treatment journey. Her story is one example of a wider shift in healthcare: toward patient-centred care — an approach that puts the individual’s needs, values, and context at the heart of decision-making.
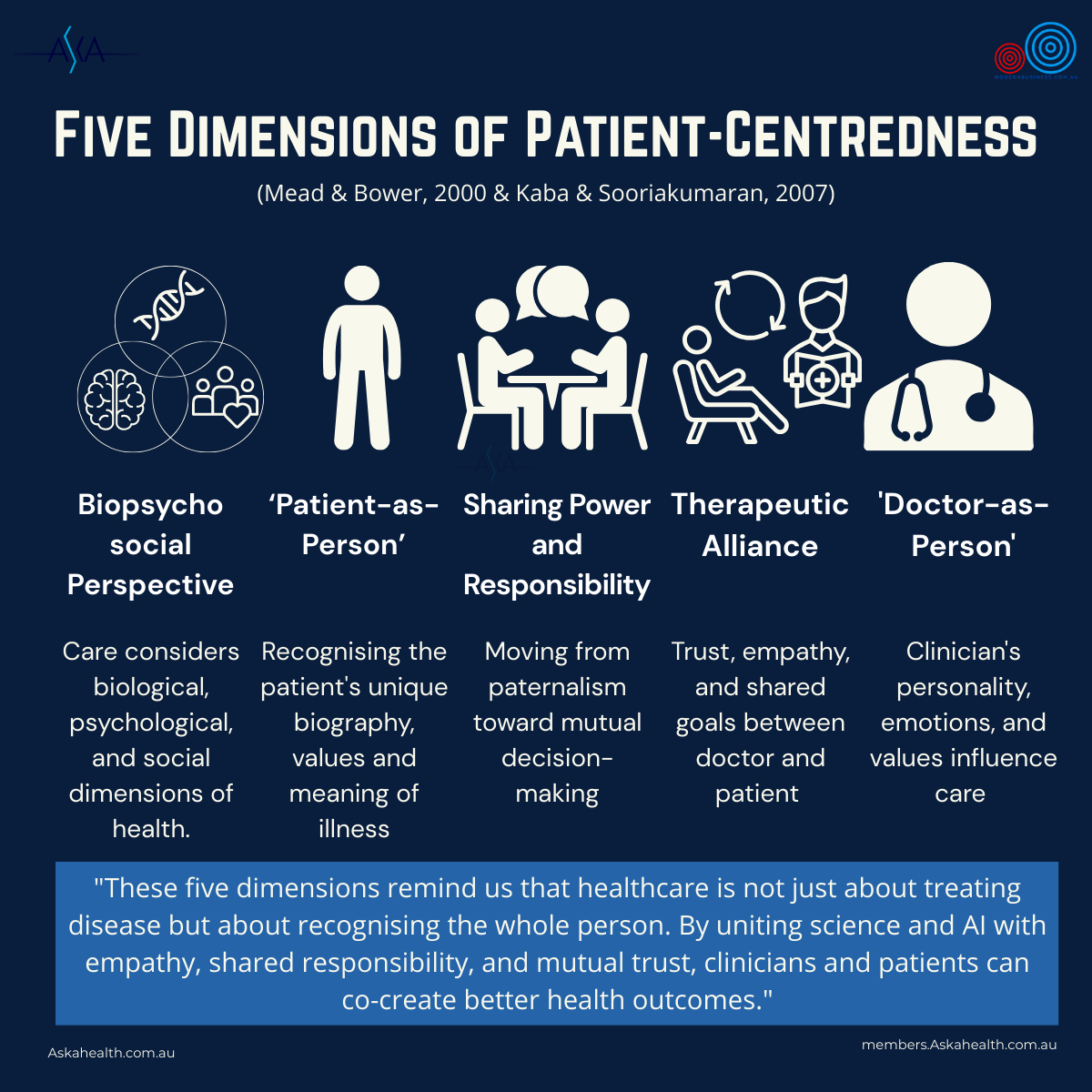
To understand what “patient-centred” really means, we can turn to one of the most widely recognised frameworks: Mead and Bower’s Five Dimensions of Patient-Centred Care (2000). This framework describes five dimensions that together define what good practice looks like, as shown in the figure above:
- Biopsychosocial perspective – Health is shaped by biological, psychological, and social factors.
- Patient-as-person – Care recognises the individual’s biography, values, and goals.
- Sharing power and responsibility – Care is based on mutual decision-making rather than paternalism.
- Therapeutic alliance – Care depends on trust, empathy, and shared goals between patient and clinician.
- Doctor-as-person – Clinicians’ personalities, values, and humanity also shape the care experience.
Now, let’s explore how each of these dimensions played out in Carolina Millon’s journey — and how AI supported her along the way.
go to: | Start | Top of This Section | End
2. Applying the Five Dimensions to Carolina’s Case
📌 Note: If you haven’t read Blog 1 in this series, we recommend starting there to familiarise yourself with Carolina’s case. It provides the background to the patient journey we’ll be using here to illustrate each dimension of patient-centred care.
2.1 Biopsychosocial Perspective in Carolina’s Case
Carolina’s experience illustrates the interplay between biology, psychology, and social context. When her biopsy result arrived, she understood only the words “invasive carcinoma.” The rest was overwhelming jargon. AI provided an immediate translation into plain language, reducing her psychological stress and enabling her to explain the diagnosis to her family with confidence. This integration of biological data, emotional response, and social communication reflects the biopsychosocial model in action.
2.2 Patient-as-Person in Carolina’s Case
Carolina was not just a “cancer patient” — she was also a mother, partner, and professional. Patient-centred care recognises this individuality. By using AI to explore treatment information, she could weigh medical options against what mattered most to her: maintaining quality of life and being present for her children. The tools gave her the confidence to frame choices in terms of her own values.
2.3 Sharing Power and Responsibility in Carolina’s Case
When her clinicians presented differing views on radiation therapy, the old model might have left Carolina confused and passive. Instead, she used AI to review evidence-based pros and cons. This enabled her to actively contribute to the decision-making process. She didn’t make the choice alone — but she wasn’t sidelined either. The balance of power shifted toward genuine collaboration.
2.4 Therapeutic Alliance in Carolina’s Case
Trust and empathy are essential for good care. By arriving informed, Carolina made consultations more productive: less time was spent decoding medical terms, and more time on addressing concerns and planning next steps. This strengthened the therapeutic alliance, allowing her doctors to engage with her as a knowledgeable partner rather than a passive listener.
2.5 Doctor-as-Person in Carolina’s Case
Clinicians bring more than technical expertise; their personalities and values also shape care. In Carolina’s case, AI freed her doctors from lengthy explanations of technical jargon, giving them more space to bring empathy, reassurance, and nuance into the consultation. AI acted as a supportive layer, not a substitute, allowing the doctor’s human qualities to shine.
go to: | Start | Top of This Section | End
3. Summary Table: Carolina’s Case Across the Five Dimensions
| Dimension | Description | How It Appeared in Carolina’s Case |
|---|---|---|
| Biopsychosocial perspective | Health includes biological, psychological, and social aspects | AI clarified jargon, reducing stress and helping her explain results to family |
| Patient-as-person | Recognising the individual’s values and goals | Carolina weighed treatment choices against her priorities as a mother and professional |
| Sharing power and responsibility | Decisions are made collaboratively | AI helped her compare treatment options and join in decision-making |
| Therapeutic alliance | Care built on trust and empathy | Consultations focused on planning and concerns, not just definitions |
| Doctor-as-person | Clinician’s humanity shapes care | AI freed doctors to focus on empathy and reassurance |
go to: | Start | Top of This Section | End
4. Why Carolina’s Case Matters
Carolina’s journey is not just one patient’s story. It’s a demonstration of how the Five Dimensions of Patient-Centred Care can come alive in everyday practice. With AI as a supportive tool, patients can enter consultations informed, ask better questions, and share responsibility for decisions. Doctors, in turn, can focus more on empathy, trust, and partnership.
AI doesn’t replace the human relationship. It strengthens it — by ensuring both patients and clinicians share the same foundation of understanding
go to: | Start | Top of This Section | End
Research Evidence
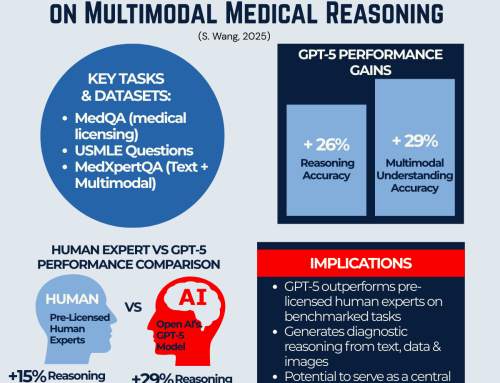
Recent research on GPT-5’s multimodal medical reasoning capabilities shows that the latest generation of AI can integrate text, structured data, and medical images to produce reasoning that, in benchmark tests, surpasses pre-licensed human experts.
This supports the application of patient-centred care principles in the digital age — giving patients the ability to understand complex medical information and actively participate in decisions across all five dimensions.
📄 Read our full review here: Breaking Barriers: How GPT-5 is Advancing Multimodal Medical Reasoning Beyond Human Expertise
go to: | Start | Top of This Section | End
Relevant Blogs in This Series
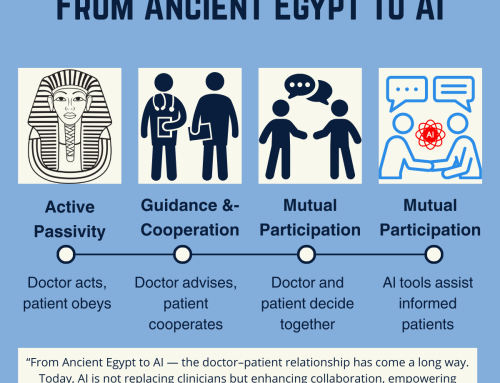
👉 If you’re ready to continue, Blog 3 traces the historical evolution of the doctor–patient relationship — from Ancient Egypt to AI.
Here’s what’s next:
- From Patients to Partners — How informed patients like Carolina Millon are reshaping care.
- The Five Dimensions of Patient-Centred Care. (This Blog)
- From Ancient Egypt to AI — The fastest leap in the doctor–patient relationship in history.
- Breaking Barriers — How GPT-5 is advancing multimodal medical reasoning beyond human expertise.
- From Patients to Partners — AI’s real-world impact on healthcare.
- Understanding the Patient Journey — A new framework for communication in modern healthcare.
🌍 We hope this series will serve as a mini masterclass for practitioners and healthcare innovators — helping to reimagine healthcare and shape it for the better.
💬 Before you move on, we’d love to hear from you:
Your feedback will help us refine and shape the rest of this series to provide even more value for medical practices. Please scroll down and share your comments below.
What stood out most for you in this article?
- Did Carolina’s case change how you think about patient-centred care?
- Which of the Five Dimensions feels most relevant in your work today?
- Where do you see AI helping (or hindering) in practice?
Scroll down & please share your perspective in the comments below. Your insights will help shape this series and spark a richer dialogue for all of us.
go to: | Start | Top of This Section | End
Join the Movement
If this series of blogs has sparked your imagination about how healthcare delivery could be transformed — making it more accessible, affordable, and equitable while also reducing burnout among healthcare professionals — we invite you to connect with the Co-Create Care Movement.
This growing community brings together healthcare innovators, leaders, clinicians, and forward-thinkers who are exploring how AI can be used responsibly to empower patients, support clinicians, and improve outcomes.
Connect with Co-Create Care movement.
→ Facebook Group: Aligning for Excellence
→ Community Link – Meetup Discussions @ AI in Practice (Our Fortnightly Online forum for live discussions)
Together, we can shape a future where healthcare isn’t just sustainable—it’s remarkable.
go to: | Start | Top of This Section | End
Reference
Mead, N. and Bower, P. (2000). Patient-centredness: a conceptual framework and review of the empirical literature. Social Science & Medicine, [online] 51(7), pp.1087–1110. doi:https://doi.org/10.1016/s0277-9536(00)00098-8.(Accessed: 11 August 2025)
Kaba, R. and Sooriakumaran, P. (2007). The evolution of the doctor-patient relationship. International Journal of Surgery, [online] 5(1), pp.57–65. doi:https://doi.org/10.1016/j.ijsu.2006.01.005.(Accessed: 11 August 2025)
OpenAI (2024) Introducing GPT-5 [YouTube video]. Available at: https://www.youtube.com/live/0Uu_VJeVVfo?t=2075 (Accessed: 11 August 2025). Segment: 34:35–40:55.
go to: | Start | Top of This Section | End





Leave A Comment